Conversation between customer and employee.

Are you leveraging AI to automate insurance tasks?
Discover our new, groundbreaking AI-powered transcription service for calls.
Challenges and needs
Insurance companies handle a high volume of daily phone inquiries, from claims reporting to advisory services and status requests. At the same time, there are strict requirements for documentation, compliance, fast case handling, and customer experience.
Key challenges:
- Incomplete documentation of claim details and verbal agreements.
- Time-consuming manual creation of claim cases and follow-up processes.
- Difficulty identifying patterns in inquiries or detecting potential fraud.
- Inconsistent quality in claims handling and customer dialogue.
- Challenges in maintaining structure and quality at scale.
Det gør ScriptIQ for dig
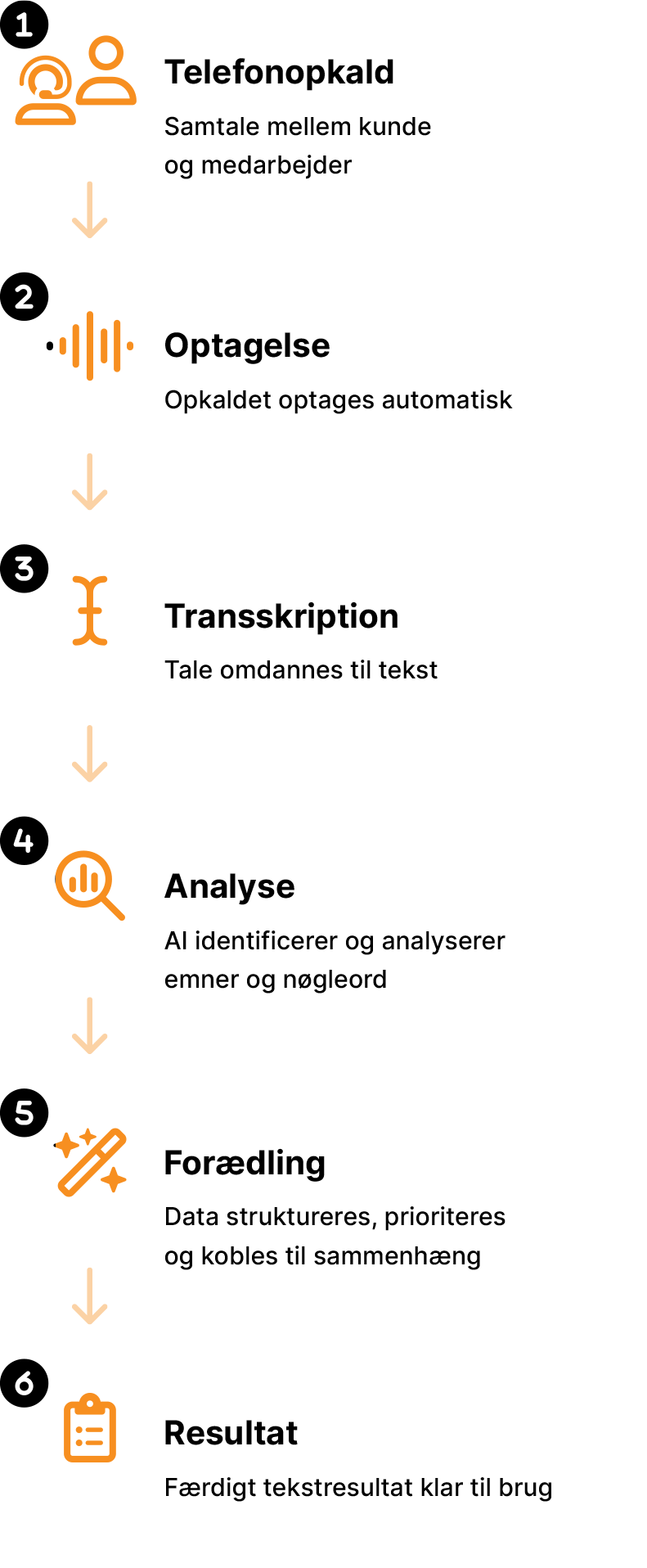
This is what ScriptIQ does for you

1. Phone call

2. Recording

3. Transcription
Speech is converted into text using AI.

4. Analysis
AI identifies and analyses topics, keywords, and content in the conversation.

5. Refinement
Data is structured, prioritised, and placed in the right context.

6. Result
A finished text output, ready to use in your daily work.
What you do
The finished text output from ScriptIQ can be delivered to you in three ways. choose the option that suits you best. from there, you can process and use the text in the way that best fits your business.

Dstny’s AI-powered transcription service, ScriptIQ
ScriptIQ converts customer conversations into text and automatically analyses and refines it into structured, final documentation. It can be used to create cases, document claims, and ensure accurate follow-up and compliance.
Practical features tailored for insurance companies:
- Automatic documentation and note-taking
AI creates structured notes that can be used for case management, documentation, and as a supplement to customer follow-up. - Automatic claims case creation
Conversations are analyzed and converted directly into a claim report with the necessary details, such as claim type, date, amount, location, and involved parties. - Customer follow-up and status emails
AI automatically generates emails or SMS messages with confirmation, next steps, and contact information. - Fraud detection and pattern recognition
AI identifies unusual phrasing, frequency, or inconsistencies that may indicate attempted insurance fraud. - Training and quality assurance
Conversations are analyzed for tone, information delivery, and process accuracy—supporting coaching and standardization.
Potential benefits with ScriptIQ
Value for insurance companies
AI-powered transcription optimizes operational efficiency, risk management, and customer experience:
Automation of claims handling
- Faster and more accurate case creation.
- Consistent and complete data capture from the first point of contact.
Stronger compliance and quality
- All conversations are documented in a structured and secure manner.
- Easy access to case history and notes throughout the entire claims process.
Intelligent risk management
- AI helps identify patterns, fraud indicators, and recurring issues.
- Proactive insight into trends and evolving customer needs.
Improved customer service and experience
- Automatic confirmations and follow-ups increase customer confidence and trust.
- Time savings enable staff to serve more customers, more effectively.
Efficient onboarding and quality control
- New claims handlers learn through real-life examples and realistic cases.
- AI-based feedback enables continuous improvement.
Potential practical use cases with ScriptIQ

Example 1 – Automatic claim creation
- A customer calls to report water damage in their home.
- AI captures the conversation, creates the case with all necessary details, and sends confirmation to the customer via email and SMS.
- A customer requests a status update on an ongoing case.
- AI automatically sends an update including the case number, contact person, and expected response time.
- AI detects that the same customer has reported similar claims three times within two months.
- The system flags the case for manual review by the claims manager.

Financial benefits
- Up to 30% faster claims processing through automatic case creation.
- Significantly fewer errors and missing information in cases.
- Reduced fraud-related payouts through early detection and alerts.
- Increased customer satisfaction and lower churn due to fast and transparent communication.
- Reduced pressure on customer service and claims handlers → higher efficiency and improved job satisfaction.